Introduction:
The frequency of pleural tumors increases constantly. Nowadays they are the subject of daily surgical interventions in every major hospital.
In this anatomic area are seen a little primary tumors, the most common from all is malignant pleural mesothelioma (MPM). Numerous malignant tumors with different histogenesis metastasize predominantly in pleura. This variety of malignant tumors requires their differentiation mainly with mesothelioma of the pleura – tumor with high malignancy and very poor prognosis. In most of the cases MPM has a structure that resembles epithelial tumor with adenomatous morphology. That’s why they can be easily mistaken with metastatic adenocarcinomas with different primary localization in the routine practice.
Although the progress of clinical, paraclinical and morphological methods the diagnosis of MMP continue to be difficult. It is an important issue in the diagnostic histopathology because of the progress of surgical treatment and the usage of more effective chemo – and radiotherapy. The correct diagnosis is an essential condition that defines the proper treatment and prognosis for the patient.
Materials and methods:
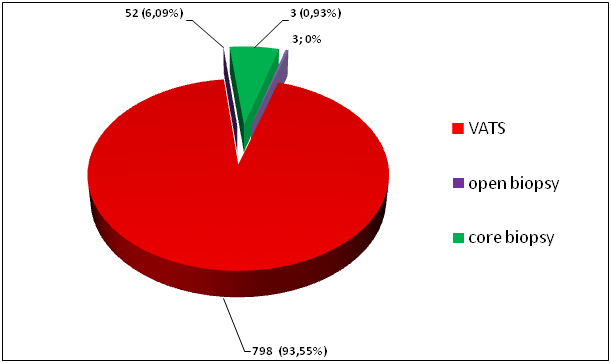
853 cases of pleural materials were histologically investigated. Biopsy material from pleura can be taken by several methods: core needle biopsy – 3 cases (0,35%) and open biopsy – 42 cases (4,92%). In the rest 828 (97,06%) cases the material is taken by VATS. (fig. 1)
Fig. 1. Distribution of the histological material according to the biopsy type
Macroscopic assessment of the biopsy material taken by VATS showed that in 743 (93,1%) cases it was presented by single fragments with the shape of cube and size of each side about 0,5 cm. In all other 55 (6,9%) cases the material was larger. This material was enough for histological investigation. Only 8 cases (0,93%) were assessed as inadequate for diagnosis and rebiopsy was recommended. 21 (2,82%) of the cases were with damaged edges and significant crush phenomenon caused by taking the material.
Urgent intraoperative biopsy consultation is widespread in the diagnosis of tumors of the pleura. According to our results it was done in 379 cases, represented 44,43% of all histological materials. They included both tumors and non tumors of the pleura. From them clinically diagnosed non tumors were 168 (44,32%) cases, and tumors were 211 (55,68%) cases. The comparison between diagnosis placed by urgent intraoperative biopsy consultation and the one made by the final histological material enable us to make conclusion for the diagnostic value and accuracy of frozen section investigation. Tumors are divided in two groups – malignant mesothelioma and metastatic tumors of the pleura. This allow to check the accuracy of intraoperative biopsy consultation in different difficult diagnosis. We use the results from the final histological examination and observe their match or mismatch with frozen section investigation. From all 379 intraoperative biopsy consultations, tumor processes are 182, non tumor diseases are — 168, and МPM – 30.
Table 1 show the summarized data from all intraoperative biopsy consultations for the divided groups and statistical categories to true positive, false positive, false negative and true negative. It is seen that the results of tumors and non tumors of pleura are almost equally divided, while mesotheliomas have more false negative results.
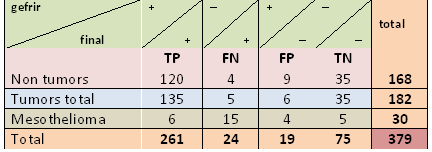
Table 1. Matches and mismatches in intraoperative biopsy consultations of pleural diseases
Legend: TP=true positive, FN=false negative, FP=false positive, TN=true negative
The results from table enable us to make a statistical analysis about diagnostic value of the frozen section investigation due to its sensitivity, specificity, maximum accuracy, positive predictive value and negative predictive value in non tumors, metastatic tumors and ММP.
We use the following statistical formulas:
- Sensitivity = (TP/ (TP+FN)) × 100
- Specificity = (TN/ (TN+FP)) × 100
- Accuracy = [(TP+TN)/ (TP+TN+FP+FN)] × 100
- Positive predictive value PPV = (TP/ (TP+FP)) × 100
- Negative predictive value NPV= (TN/ (TN+FN)) × 100
Results:
The received results show that in non tumors the intraoperative biopsy consultation is a method with increased limit accuracy – 92,26%, good positive predictive value 93,02% and negative predictive value is 89,74%. Sensitivity of the method for this group of diseases is 96,77% and specificity is 79,54%.
In metastatic tumors the results from statistics are similar – accuracy of the method 93,92%, PPV=95,74%, NPV=68,74%. The sensitivity of express intraoperative consultation is 96,42, and the specificity is – 85,36%.
We used intraoperative biopsy consultations in 30 cases of malignant mesothelioma, which was 60,00% from all 50 cases of such tumors. The maximum accuracy of the method was decreased – 36,66%, with low NPV — 25%, and average PPV – 60%. Sensitivity and specificity of the urgent intraoperative biopsy consultation of mesothelioma were decreased – 28,57% and 55,55%. Confirmatory diagnosis of mesothelioma was placed by using intraoperative biopsy consultation in only 6 cases from 30 examinations. (13,95%).
Figure 2, show the results about diagnostic accuracy, sensitivity, specificity, predictive positive value and negative value for non tumors, metastatic tumors and malignant mesotheliomas.
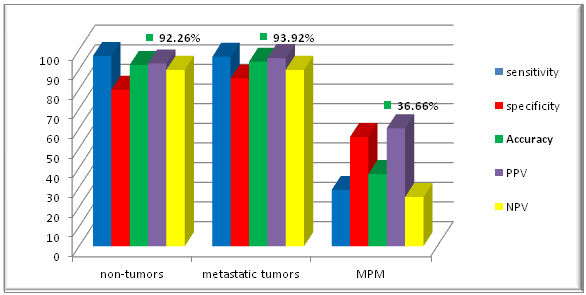
Fig. 2. Diagnostic value of frozen section for non tumors, metastatic tumors and malignant mesothelioma
The correct pathological diagnosis of mesothelioma and its distinction from metastatic tumors of pleura requires investigation of tissue biopsy material. VATS is preferred method of taking pleural material. The received material is enough in 98% of the cases for a further histological and immunohistochemical examination.
Intraoperative biopsy consultation has decreased sensitivity and specificity and is not recommended for diagnosis of МPM, especially in the presence of a small, single material.
Discussion:
The main reasons for performing intraoperative biopsy consultation, also called frozen section ( FS ) are: to establish the presence and nature of a lesion, to determine the adequacy of surgical resection margins, and to establish whether the tissue obtained contains enough diagnosable material for microscopic examination. Furthermore, the analysis of the accuracy of the method (frozen biopsy) is extremely important in order to minimize inadequate surgical procedures. [4, с. 149] The accuracy of frozen section examination varies according to the specific anatomical site that is examined which ends up interfering directly in the global diagnostic accuracy of a service. [8, c.337], [1, c.469], [5, c.1137]
The accuracy rate of FS constitutes an important step of quality assessment step in pathology practice. A correct diagnosis principally requires good technique followed by a meticulous examination. Because the examination techniques of each pathology department may differ from one another, the comparative examination of frozen sections and routine sections would aid in becoming familiar with various pathologies and would be beneficial for pathologists in minimizing their diagnostic errors.
According to a large study for 5 years period, Renata and collaborators report that urgent intraoperative biopsy consultation of pleural materials is used in only 15 cases which is about 0,5% from all biopsies and the correct diagnosis is placed in 86% of the cases. [9, c. 387]
The results from Akyildis, are similar. It report that from 25 frozen section materials of the pleura, 11 /44%/ are with wrong diagnosis, without specifying the numbers of false negative and false positive. The wrong frozen section diagnosis were mainly in diagnostic of malignant mesothelioma and its distinguishing with metastatic pleural tumors. There are only single wrong intraoperative biopsy consultations in distinguishing of MMP and benign mesothelial proliferation or tumor necrosis that are assessed as granulomas with necrosis. [2, c.7961]
In other small series composed of 20 intraoperative biopsy consultations – 10 of each benign lesions and 10 metastatic tumors was reported that in all benign lesions frozen section diagnosis was confirmed by investigation of paraffin sections and tumors in 60%. This warrants that the method was felicitous in the performance of pleurodesis but quite insecure to define the volume of surgical intervention in malignant lesions of the pleura. [6, c 636]
We analyse the usage of frozen section investigation only in one anatomical area which is rare because of the specifics of surgical interventions and the way of receiving tissue material. We use intraoperative biopsy consultation a lot and it is widespread in diagnosis of pleural tumors due to the presence of Department of Thoracic Surgery in our University hospital.
Most of our biopsy materials (97,06%), are received by the usage of VATS. According to most authors VATS is preferred method for taking a biopsy from the pleura. The received material is enough for histological and immunohistochemical examination in 98%. This statement is supported and from other authors [3, 6 c.636]
Our results are based on a huge number of intraoperative biopsy consultations — 379 cases, that presents 44,43% from all histological materials. We use objective statistical processing of the data to define the diagnostic value of intraoperative biopsy consultation. They show that in tumors and non tumors of the pleura FP и FN results are almost equally divided while in malignant mesothelioma there are three times more FP results. This give us a reason to accept that frozen section investigation is with increased accuracy, sensitivity and specificity and we can use it in all benign lesions of pleura.
The results from the statistical processing of metastatic pleural tumors are similar – increased accuracy, sensitivity and specificity and this makes the usage of the method effective.
The situation with diagnosis and assessment of the surgical intervention in MMP is not the same. Statistical processing of the received data for this tumor show decreased accuracy, sensitivity, specificity and diagnosis of mesothelioma is placed only in 6 cases from 30 cases (13,95%). This allow us not to recommend the urgent intraoperative biopsy investigation when there is a clinical diagnosis – MMP. It is related with high value of false negative results.
Conclusion:
Urgent intraoperative biopsy consultation of MPM has decreased accuracy, sensitivity and specificity and it is not recommended for the correct diagnosis, especially on a single material.
Frozen section investigation of non tumors of the pleura is a method with increased accuracy and good predictive positive value. Sensitivity and specificity of the method are also increased and its usage is recommended.
In metastatic pleural tumors the results from statistical processing are similar – increased accuracy, sensitivity and specificity and that supports the usage of intraoperative biopsy consultation as an effective method.
REFERENCES:
- Ahmad Z, Barakzai MA, Idrees R, Bhurgri Y. Correlation of intraoperative frozen section consultation with the final diagnosis at a referral center in Karachi, Pakistan. Indian J Pathol Microbiol 2008; 51(4):469-73.
- Akyildiz EU. Intraoperative pathology consultation for pulmonary lesions: errors and deferrals. Int J Clin Exp Pathol 2015;8(7):7961-7966
- Cagle P.T. and T.C. Allen, Frozen Section Library: Pleura, Frozen Section Library 3, Springer Science + Business Media, 2010
- Da Silva RD, Luís RS, Graziela DM.et al. Diagnostic accuracy of frozen section tests for surgical diseases. Rev. Col. Bras. Cir. 2011; 38(3): 149-154
- Ferreiro JA, Myers JL, Bostwick DG. Accuracy of frozen section diagnosis in surgical pathology: review of a 1-year experience with 24,880 cases at Mayo Clinic Rochester. Mayo Clin Proc 1995; 70: 1137-1141.
- Fielding D, Hopkins P, Serisier D. Frozen section of pleural biopsies at medical thoracoscopy assists in correctly identifying benign disease. Respirology.2005 Nov;10(5):636-42.
- Oviedo SP, Philip TC. Diffuse Malignant Mesothelioma Arch Pathol Lab Med. 2012; Vol 136:882-888
- Raab SS, Tworek JA, Souers R, Zarbo RJ. The value of monitoring frozen section-permanent section correlation data over time. Arch Pathol Lab Med 2006; 130(3):337-42.
- Renata Langfort, Ewa Szczepulska-Wójcik, Piotr Rudziñski, Tadeusz Orowski. Evaluation of frozen section usefulness for the diagnosis of pulmonary lesions, pleural and mediastinal diseases, for the detection of metastasis of lung cancer in mediastinal lymph nodes, and for the assessment of surgical margins in lung cancer resection specimens. Kardiochirurgia i Torakochirurgia Polska 2007; 4 (4): 387–396[schema type=»book» name=»DIAGNOSTIC VALUE OF FROZEN SECTION DIAGNOSIS OF PLEURAL DISEASES» description=» Objective: Urgent intraoperative biopsy consultation is widespread in diagnosis of pleural tumors. Our aim is to evaluate the accuracy of frozen section investigation of pleural diseases. Materials and methods: We conducted a retrospective study from a database of frozen section investigations of pleural materials. There were examined 379 cases, which represented 44,43% of all histological materials. From them non tumors were 168 (44,32%), and tumors were 211 (55,68%). The materials were divided into three groups: non tumors, metastatic tumors and malignant pleural mesothelioma (MPM). These diagnoses were compared to definite paraffin, used as controls and “golden standard”. The coincidence of diagnosis placed by frozen section investigations and one placed by final histological materials enable us to divide them into true positive, false negative, false positive and true negative. This allow us to make statistical analysis of diagnostic accuracy of the method due to its sensitivity, specificity, maximum accuracy, positive predictive value and negative predictive value. Results: Frozen section investigation of non tumors is a method with increased accuracy – 92,26%, and good predictive positive value /PPV/ — 93,02%. Sensitivity of the method is 96,77%, and specificity — 79,54%. The statistical results for metastatic tumors are similar – accuracy of the method- 93,92%, PPV=95,74%, NPV=68,74%. Sensitivity of the intraoperative biopsy consultation is 96,42, and specificity – 85,36%. Urgent intraoperative biopsy consultation was done in 30 cases of MPM, which was 60,00% from all such 50 tumors. The maximum accuracy of the method was decreased – 36,66%, with low NPV — 25%, and average PPV – 60%. The sensitivity and specificity of the frozen section was decreased – 28,57% and 55,55%. Confirmatory diagnosis of mesothelioma was placed only in 6 cases from all 30 (13,95%). by using frozen section investigation. Conclusions: Urgent intraoperative biopsy investigation is accurate enough and is recommended for diagnosis of non tumors and metastatic tumors of pleura. Frozen section investigation has decreased sensitivity and specificity and is not recommended for diagnosis of MPM, especially on a single material.» author=»Peshev Zhivko Vladimirov, Koleva Mariya Stoyanova, Dikov Dorian» publisher=»БАСАРАНОВИЧ ЕКАТЕРИНА» pubdate=»2016-12-23″ edition=»euroasian-science.ru_25-26.03.2016_3(24)» ebook=»yes» ]